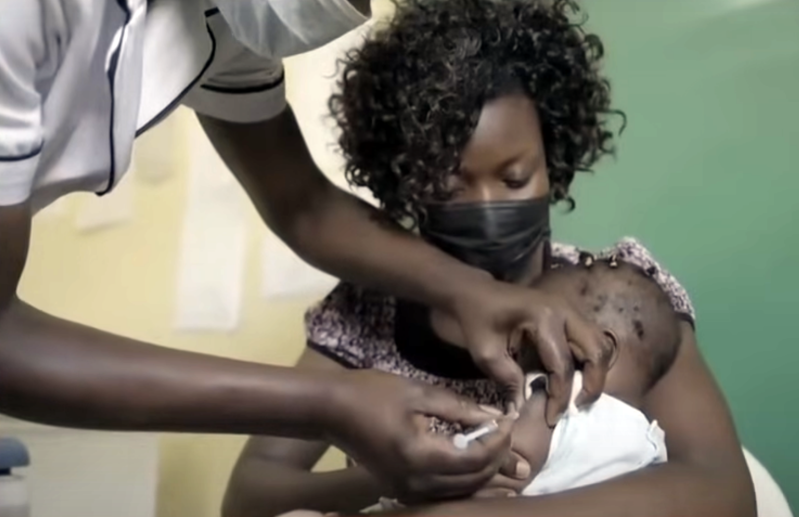
Cameroon has become the first country to launch the much-anticipated malaria vaccine amidst public skepticism on its efficacy and safety. Despite the initial vaccine hesitancy from the public, the World Health Organisation (WHO) has termed the malaria vaccine mass rollout in Cameroon as ‘a significant step’ in the prevention of the disease. Baptist churches have come alongside to play an important role in helping to counter misinformation and build trust among grassroot communities.
The central African country took the bold step to include the WHO-approved malaria vaccine into its routine immunization program. From January 22, children under six months have been getting free doses of the RTS,S malaria vaccine alongside other vaccines such as polio, measles, tetanus and meningitis.
The disease, caused by parasites found in infected female Anopheles mosquitoes, killed over 600,000 people in 2022, according to WHO. 95 percent of the deaths were registered in Africa and among those, about 80 percent were children under 5 years.
Cameroon’s pioneer malaria vaccination programme will provide critical lessons for other African high-risk countries such as Liberia, Niger, Burkina Faso and Sierra Leone that are due to receive over 1.7 million doses of the vaccine in the coming months.
The journey to developing a WHO-approved malaria vaccine has been long and arduous but well worth the effort following successful clinical trials and pilot phases.
The vaccine, which has been developed over 30 years by pharmaceutical giant GSK, showed an efficacy rate of 40 to 50 percent. Compared to the Covid-19 vaccines, which have an efficacy rate of over 90 percent after the second dose, this could be deemed as low. Nevertheless, scientists are in agreement that the malaria vaccine adds another important layer of protection and should be used alongside insecticide-treated mosquito bed nets, periodic antimalarial drugs and insecticide spraying during rainy seasons.
If sustained, these interventions have the potential to significantly reduce and even eliminate malaria in more countries. Cape Verde, a small archipelago nation off the coast of Senegal, is a case in point. Through a multi-pronged strategy of spraying insecticide targeting mosquito larvae in breeding grounds and early detection and efficient management of cases, the WHO declared the country malaria-free last month after attaining zero infections for three consecutive years. Cape Verde joins Algeria and Mauritius who were declared malaria-free in 2019 and 1973 respectively.
Similar interventions have seen a reduction of local infections in Eswatini (57.6 percent), South Africa (31.3 percent) and Botswana (43.5 percent) in 2022. The introduction of the vaccine will further bolster the previously used interventions.
Head of malaria vaccine development at PATH, Ashley Birkett, says reducing infections by 30 percent translates into saving thousands of lives.
“In one of the clinical centres involved in the phase 3 trial, we saw over 6,000 cases of malaria prevented for every 1,000 children who were vaccinated,” Birkett noted, implying that the vaccine mitigated against malaria multiple times for some children.
The results of a pilot phase carried out in 2019 in Ghana, Kenya and Malawi provided broader evidence of including the vaccine as part of the immunization programme. Over 830,000 children in the three countries received three doses of the vaccine reducing cases of severe malaria by 30 percent.
Dr. Bernhards Ogutu, the Chief Research Officer at the Kenya Medical Research Institute (KEMRI) and part of the Malaria Clinical Trials Alliance told Christian Daily International that the vaccine proved to be both effective and cost effective.
“Greater benefits of the vaccine are observed over a longer period. The RTS,S pilot phase in the three countries took four years where we saw a reduction of infections and lower mortality rates,” explained Dr. Ogutu.
But as the scientific community and the Government of Cameroon celebrate this breakthrough, another battle is being fought: that against misinformation spreading mainly on social media. The Vaccine Alliance (GAVI) reports that a significant number of Cameroonians are skeptical about the efficacy and safety of the vaccine despite reassurance from government officials including the Minister of Public Health, Dr. Manaouda Malachie.
“The process of introducing this vaccine followed all the essential required steps, including the approval of the National Immunization Technical Advisory Group,” assured Dr. Malachie in a press statement.
The Cameroonian government has identified and is rolling out public awareness programmes with local and regional partners as one of the ways to counter the vaccine disinformation.
One of the key partners in creating awareness of the vaccine and mobilizing the community is the Cameroon Baptist Convention through its CBC Health Services Malarial Control and Prevention program. The program aims to accelerate progress towards the elimination of malaria by “addressing barriers such as resistance to change, inadequate knowledge among stakeholders, insufficient capacities of community stakeholders for effective strategies in communication, education and advocacy.”
Through its assemblies, schools and hospitals, the Baptist Church holds significant influence in Cameroon.
Professor Tih Pius Muffih is the Director of Cameroon Baptist Convention Health Services. He urges parents to embrace the vaccine without fear and projects a significant reduction of malaria cases in children.
“The vaccine will not only mitigate the impact of malaria in the country but also reduce expenses related to preventing or treating this disease,” he says.
Estimates published by the Malaria Journal estimates that Cameroon spends up to US$3.88 monthly per capita in malaria prevention and treatment, costs that could go to better use if the vaccine and other interventions work to significantly reduce prevalence of malaria.






